Does work time limit for resident physician affect short-term treatment outcome and hospital length of stay in patients with spontaneous intracerebral hemorrhage?: a two-year experience at a single training hospital in South Korea
Article information
Abstract
Objective
To compare short-term treatment outcomes at hospital discharge and hospital length of stay (LOS) in patients with spontaneous intracerebral hemorrhage (sICH) before and after introduction of resident physician work time limit (WTL).
Methods
We retrospectively reviewed consecutive patients treated for sICH at our institution between 2016 and 2019. Then we dichotomized these patients into two groups, pre-WTL and post-WTL. We analyzed demographic elements and clinical features, and hospital length of stay (LOS). We evaluated short-term outcome using modified Rankin scale score at hospital discharge and then divided it into “good” and “poor” outcome groups. We subsequently, compared short-term treatment outcome and hospital LOS between the pre-WTL and post-WTL groups.
Results
Out of 779 patients, 420 patients (53.9%) were included in the pre-WTL group, and 359 (46.1%) in post-WTL. The mortality rate in sICH patients was higher in the post-WTL group (pre-WTL; 13.6% vs. post-WTL; 17.3%), but there was no statistically significant difference in short-term outcome including mortality (p=0.332) between the groups. The LOS also, was not significantly different between the two groups (pre-WTL; 19.0 days vs. post-WTL; 20.2 days) (p=0.341). The initial Glasgow Coma Scale score, personal stroke history, and mean age were the only independent outcome predicting factors for patients with sICH.
Conclusions
Some neurosurgeons may expect poorer outcome for sICH after implementation of the WTL of the K-MHW for resident physician however, enforcement of the WTL did not significantly influence the short-term outcome and hospital LOS for sICH in our hospital. Further well-designed multi-institutional prospective studies on the effects of WTL in sICH patient outcome, are anticipated.
INTRODUCTION
From ancient civilization, medicine in general have concerned about patient treatment outcome, patient safety, and medical education and training of the trainee. And in certain aspect, every kind of work time limit (WTL) for trainee itself might amplify these concerns. The WTL enacted by the Korea’s ministry of health and welfare (K-MHW) for resident physician had an officially legal validity since March 1, 2018 in South Korea after an optional trial for a few months. Similar regulations were adopted in the United States (US) in 2003 and in the European Union (EU) in 2008 after a long preparatory term of at least 10 years [9,27].
A one-size-fits-all approach, however irrespective of medical specialty, to patient care and resident education with practical training have not always been welcomed by both the faculty and resident physician in training hospital. Then, in the US and a few EU countries there have been a number of issues and debates before and after the implementation of their WTL with regard to patient safety, treatment outcome, resident fatigue, wellbeing, training, on-duty pattern, and performance. Most studies on these topics have reported unclear research results in the last two decades, especially those on patient treatment outcome [5,7,11,13,23,38].
The primary goal of the present study was to compare short-term treatment outcome at hospital discharge in spontaneous intracerebral hemorrhage (sICH) patients before and after the enforcement of WTL by the K-MHW for resident physician at a single training hospital. There were six resident physicians within the Department of Neurosurgery and the number has been constantly maintained throughout the study period. Also, the total numbers of intensivists and nursing staffs working for the department of neurosurgery were remained identical throughout the study period. The authors never have had any physician assistant, neurointerventionalist, or fellow neurosurgeon until today.
MATERIALS AND METHODS
This study was approved officially (GBIRB2020-141) by the institutional review board (IRB) at the authors’ hospital. This study also, was exempted from the informed consents for included patients by the IRB.
Korea’s WTL for resident physician
Actually, the authors of this study could not find out any written and formal papers within the Department of Neurosurgery on the past regulations of resident work hour restriction before commencing the central government WTL for resident physician. The rules for resident work hour had been self-regulated by the department’s resident physicians including the chief resident for maintenance of high-quality patient management and training of themselves, and the director of the resident training program had approved the rules considering the didactic and clinical educations of the trainees.
The regulations of K-MHW WTL on duty hour for resident physician are obligatory and the core contents of the regulations are as followings; 1) Resident physician’s on-duty hour is strictly restricted to 80 hours per week, averaged over 4 weeks, with an extension of 8 hours for educational purpose. 2) The regulations constraint resident’s duty a 36-hour limit on successive duty, with 4 more hours permitted under emergency-related situations. 3) A minimum of 10 hours of break free of the patient care is mandated between on-duty hours.
Patients
Consecutive sICH patients presenting at our hospital from January 1, 2016 to December 31, 2019 were selected and their data were arranged from the departments’ logs. The authors divided these patients into two groups. One group was composed of patients from 2016 to 2017 and was called the pre-WTL group. The other was composed of patients from 2018 to 2019 and called the post-WTL group. Patients with sICH attributed to intracranial tumor hemorrhages, hematological disorders (hemophilia, leukemia), hemodialysis for various etiologies, and other cerebrovascular diseases (e.g., ruptured cerebral arteriovenous malformation or fistula, intracranial aneurysm, cavernous malformation, angioma, telangiectasia) were excluded. We also excluded subjects who died within 6 hours of visiting the emergency department (ED). We arbitrarily divided the whole patients into two age groups, one was middle aged group (below 69 years) and the other was old age group (over 70 years).
We retrospectively reviewed the patient’s medical records, including head computerized tomography (CT) or magnetic resonance image (MRI) scans. The following demographic and fundamental clinical components of the 779 patients were included in this study: age, sex, initial Glasgow Coma Scale (GCS) score, hemorrhage location (basal ganglia, thalamus, other subcortical region, cerebellum, and brainstem), most frequent and major comorbidity history (hypertension and diabetes mellitus), health-related life style characteristics (heavy alcohol consumption [alcoholism] and cigarette smoking), personal and familial history of stroke, treatment method (craniotomy/craniectomy and hematoma removal with or without neuronavigation- or neuroendoscope-guidance, stereotactic aspiration with or without extraventricular drainage [EVD] and/or thrombolytics, and conservative management with or without intracranial pressure [ICP] monitoring), and short-term outcome of treatment at discharge from hospital (good modified Rankin scale [mRS] score [4]; 0-3, poor mRS score including dead; 4, 5, and 6). We regarded some of the enrolled patients with moribund discharges from the authors’ hospital as dead.
The demographic and fundamental clinical components described above were searched from recently published reports that commonly included age, sex, neurological grade at ED arrival, location and/or extent and pattern of sICH, personal history of stroke, comorbidity and/or health-related conditions such as hypertension, diabetes mellitus, cigarette smoking, alcoholism, and family history of stroke [19,28,29]. These factors were collected and sorted for all subjects.
We defined hypertension, diabetes mellitus, alcoholism, and cigarette smoking according to generally accepted or standardized definitions and guidelines. The initial GCS score at ED and the short-term treatment outcome at hospital discharge based on mRS score were evaluated and calculated by the resident physicians and the authors.
Management principles
First of all, exact diagnosis of sICH was formally confirmed by the absence of recent head injury and by the universally acknowledged methods including head CT, MRI, CT angiography, and MR angiography as needed. The type of treatment was chosen by the resident physicians and the authors through discussions.
The early (within 24 hours of sICH occurrence) open surgical evacuation or stereotactic aspiration of hematoma with or without EVD or ICP monitoring was carried out using neuroendoscope and/or neuronavigation when we ultimately determined surgical management to be appropriate. We considered the situation of each patient and the results of radiological examinations to tailor the type of treatment. Perioperative and conservative managements strategies such as blood pressure modulation and ICP control complied with the global standard protocols or generally accepted principles. After the decision on the type of treatment for sICH was made, all included subjects were cared for in the emergency and/or neurosurgical intensive care unit (ICU) for some time.
Assessment of treatment outcome at hospital discharge
The primary short-term outcome for sICH indicator used in this study was a level of restoration of normal cerebral functions in the activities of daily living as determined by the authors and resident physicians using the simplified mRS score scheme described above (as good and poor including dead) at hospital discharge, and the secondary outcome indicator was length of stay (LOS) in the authors’ hospital.
Some clinical variables that might have impacted the short-term treatment outcome and hospital LOS such as blood lipid levels, history of coronary or peripheral arterial disease, current administration of anti-coagulants or anti-platelet drugs, artificial ventilation during sICH management, long-lasting comorbid conditions (chronic lung, liver, and renal diseases, etc.), were not checked or recorded at ED and/or during the whole course of sICH treatment for substantial number of patients, so these parameters were exempted from this analysis.
Statistical analysis
Basic demographic and clinical variables were analyzed using the t-test, [chi]2 test, or one-way analysis of variance (ANOVA) test, as appropriate. A univariate outcome analysis was accomplished using the one-way ANOVA and [chi]2 test, and a multivariate method using logistic regression analysis. The probability value for inclusion was set at 0.05. Adjusted odds ratios (ORs) with 95% confidence intervals (CIs) were computed. A two-tailed probability value (p) of <0.05 was deemed statistically significant. All variables except age and hospital LOS were considered to be categorical variables. Statistical analysis and calculation were conducted using a commercially available statistical software package (SPSS 20.0: SPSS Inc., Chicago, IL, USA).
RESULTS
Study patients
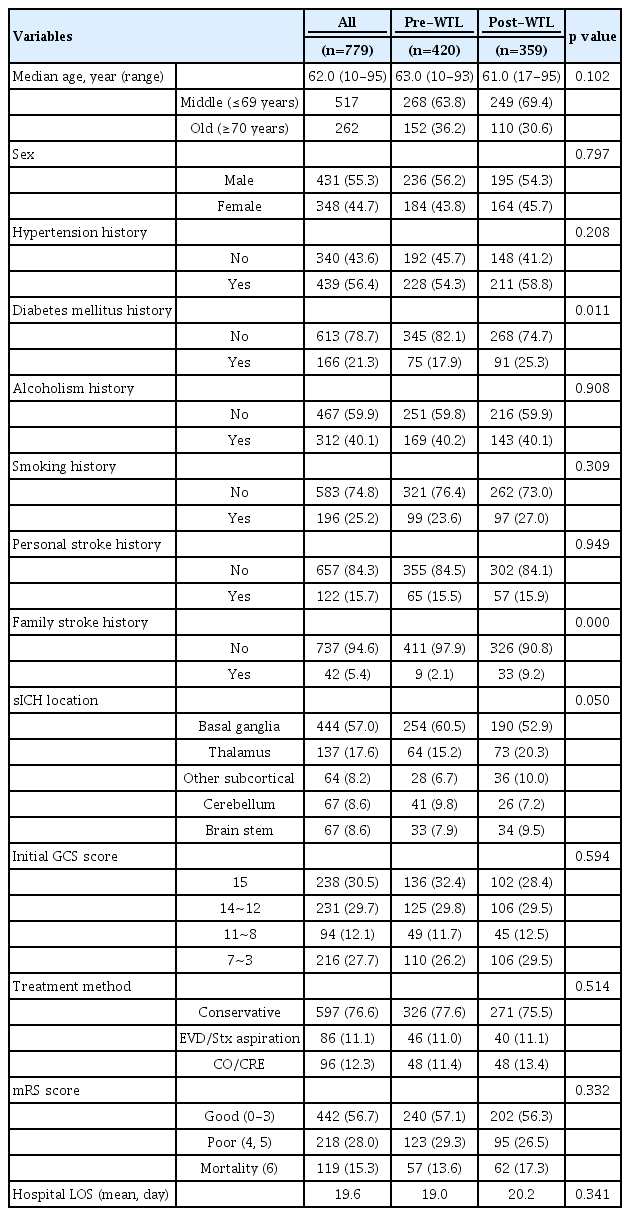
From the original 816 patients, who were admitted and treated at our hospital with a diagnosis of sICH during the study period, we excluded 37 subjects because of hemorrhages due to brain tumors, hematological disorders, hemodialysis, and other cerebrovascular diseases, or missing any data that we planned to analyze and to compare. As a result, there were 779 patients in which 420 patients were belonged to the pre-WTL group and 359 patients were the post-WTL (Table 1).
The following basic features of the 779 study subjects were saved into a data log: age, sex, initial ED GCS score, treatment type, sICH location on the head CT or MRI, simplified short-term treatment outcome at hospital discharge using the mRS score, and LOS at the hospital. A few major health-oriented risk factors that could affect treatment outcome, such as history of hypertension, stroke, diabetes mellitus, heavy alcohol consumption, cigarette smoking, and family history of stroke were also entered into the data log. These demographic and related clinical features are summarized in Table 1. The breakdown of patient number as per year of enrollment was as follows; 223 patients were included in 2016: 197 in 2017: 197 in 2018: and 162 in 2019.
All of the above-mentioned variables, except for the diabetes mellitus and family stroke history were comparable between the pre-WTL and post-WTL groups, and no significant differences were observed between them (Table 1). The prevalence of diabetes mellitus and family history of stroke were significantly higher in the post-WTL than pre-WTL group (p=0.011, p=0.000, respectively) (Table 1). We however, judged unanimously that such differences did not disturb the study aim in present analysis.
Short-term outcome and the LOS at hospital discharge
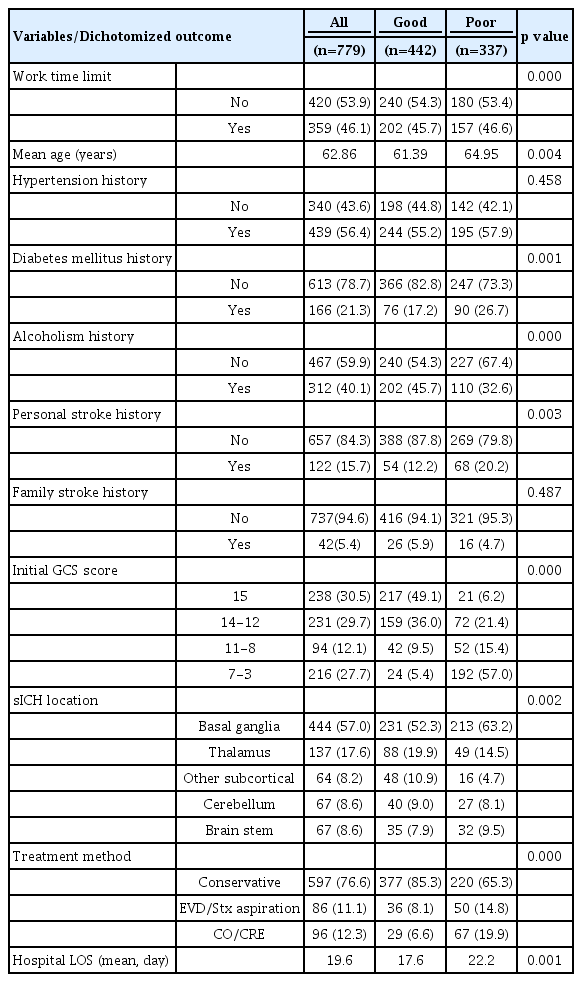
Of the 779 patients, 442 patients (56.7%) showed a good short-term treatment outcome (Table 1, 2). Table 1 demonstrates 57.1% of pre-WTL and 56.3% of post-WTL patients achieved good outcome. The good and poor (including dead), short-term treatment outcomes with their aforementioned variables are indicated in Table 2.
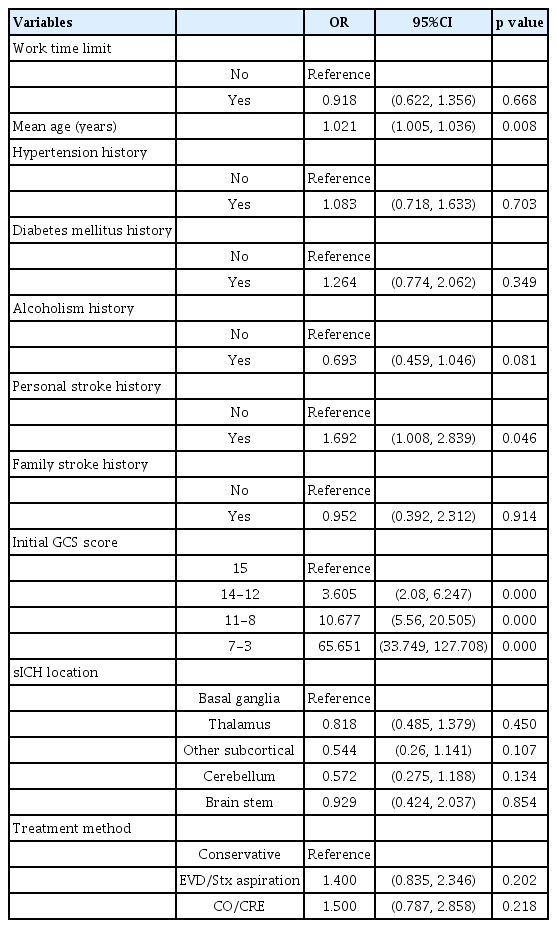
The WTL implementation, mean age, history of diabetes mellitus, prior heavy alcohol consumption, personal stroke history, initial ED GCS score, sICH location, and treatment modality showed significant difference between patients with good and poor outcomes in the univariate analysis (Table 2). On the other hand, the WTL implementation did not exert statistically significant impact on short-term treatment outcome in the multivariate logistic regression analysis (p=0.668) (Table 3). Among the various demographic and clinical variables, mean age, initial ED GCS and personal stroke history were the only predictors of short-term outcome in the multivariate analysis (Table 3).
At hospital discharge, 337 patients (43.3%) had poor short-term outcome (Table 2). A univariate analysis showed that the patients with poor short-term outcome were significantly older (mean age, 65.0 years) than those with good outcome (mean age 61.4 years) (p=0.004) (Table 2), and had significantly lower initial ED GCS scores than those with good outcome (p=0.000) (Table 2). As majority of neurosurgeon expected, a brainstem location of sICH exhibited the poorest short-term treatment outcome. Furthermore, sICH location (p=0.002) and treatment policy (p=0.000), both significantly affected the short-term treatment outcome (good or poor) in our univariate analysis (Table 2).
In a multivariate logistic regression analysis (Table 3), mean age (OR: 1.021, 95% CI: 1.005-1.036, p=0.008), initial ED GCS score (p=0.000), and personal stroke history (OR: 1.692, 95% CI: 1.008-2.839, p=0.046) were found to be significant risk factors for short-term outcome or independently and significantly predicted short-term treatment outcome. However, the WTL implementation was not verified as a significant risk factor for good or poor short-term treatment outcome (p=0.668) (Table 3). In addition, history of hypertension, diabetes mellitus, alcoholism, cigarette smoking, and family history of stroke did not appear to significantly predict short-term treatment outcome in the multivariate logistic regression analysis (Table 3).
DISCUSSION
In the US and EU wherein the WTL was implemented for resident physician much earlier than that in South Korea, enforcement of the WTL was primarily intended to reduce the resident’s sleep deficiency, to improve their clinical performance, and thereby reduce medical error and enhance patient safety [9]. Even if the national environments, policies, and cultural backgrounds in the field of medicine in South Korea have been developed quite different from those in the US and EU, the K-MHW and Korean Hospital Association (KHA) have led the resident physician’s WTL analogous to that of the US or EU, that restricted resident work hour to a maximum of 80 hours per week and 36 hours per service shift since March 1, 2018 in response to the revised Labor Standard Act.
Accordingly, each department at training hospital in South Korea has changed the service hours of the resident physicians to secure the best patient treatment outcome, and efficient and effective resident training. Now, every resident training program in South Korea has been adapted to the rules of WTL guidelines for the resident physician. Besides attaining the best patient treatment results, the faculty members of each training program in the South Korea have focused on training and education for the resident physician effectively, although the present WTL for resident physician may have some defects and/or drawbacks in terms of patient safety, patient management, and resident training.
In present study, the authors evaluated impact of the WTL for resident physician on the short-term treatment outcome including mortality rate, and hospital LOS in sICH patients through the comparison between before and after implementation of the K-MHW WTL.
Historical backgrounds of the WTL
The first case for enforcing the WTL for resident physician was based on a New York City grand jury making a decision that 18 years old Libby Zion’s death in 1984 came partially from the resident fatigue [9]. Then, in the US, the first WTL for resident physician was enacted in New York in 1989 because of concerning the patient safety [27]. In 1999, the US Institute of Medicine (IOM) claimed preventable medical errors referring that about 44,000 to 98,000 Americans die in a single year due to avoidable medical adverse events [17]. In 2003, the US Accreditation Council for Graduated Medical Education (ACGME) adopted the WTL as a common program requirement for resident physician to ensure patient and resident safety. The adoption of this guideline by the ACGME has led to gross changes in the duty hour and duty pattern of resident physician [9,12].
The ACGME’s recommendations were a 24-hour limit on successive duty, with 6 more hours permitted for transfer of care and education-related tasks, limited in-hospital call to come into force no more often than every third night, and asked a minimum of 10 hours of break between on-duty hours. Additionally, it restricted resident physician’s on-duty hours to 80 hours per week averaged over 4 weeks, with 1 in 7 days for off duty of patient management tasks [3]. The ACGME, however, changed the first version of WTL regulations in 2011 and might revise it further again in the near future [10]. Then, the ACGME regulations for the resident physician WTL are dynamic.
Patient safety, resident safety, fatigue and performance
Caruso et al. examined 48 studies on the impact of resident duty hours on patient safety and found 27 studies showing a positive effect of limiting duty hours, 17 studies showing no clear effect, and 4 studies showing a negative effect [6]. It has been demonstrated that patient safety and resident physician’s fatigue were inseparable issues because resident physician’s fatigue and/or sleep deficiency reduced the cognitive function and numerous clinical performances which might jeopardize patient safety such as medication errors [33]. At the same time resident’s fatigue and lack of sleep would also be harmful to their own quality of life (QoL) and safety, for example risk of motor vehicle accident [25].
In a few aspects, the WTL for resident physician was implemented to improve resident safety and QoL by limiting work hour. This reduction in work demands led to reduce resident fatigue and sleep deprivation, thereby also potentially reducing medical errors. Therefore, theoretically at least, the WTL might be linked directly and/or indirectly with the patient safety. There, however, have been contradictory evidences showing that the WTL for resident was not related to patient safety [12]. In 2009, Grady et al. [14] stated that there should be an adequate balance between the risk associated with resident fatigue and those associated with an inexperienced neurosurgical work force for public health. However, many researchers reported that as the WTL for resident physician has increased the number of resident hand-off and reduced practical experience, thus there were variety of concerns that the number of medical errors and complications might increase, resulting in worse patient outcome [8,9,14,16,17,20,22,24,26].
Patient treatment outcome, complication, and LOS
Clearly, resident physician’s fatigue seems to have negative influence on patient treatment outcome including complications and LOS. While enforcing the WTL for resident might have some positive effects on the treatment outcome, complication, and LOS, adverse effects due to more frequent hand-off and disruption of continuity of care were also possible [21,31]. There have been a number of literatures that the US ACGME and EU WTL’s impact on patient treatment outcome have revealed contradictory conclusions [5,7,11,23,38] and some have proved unchanged results [15,24,30,32,34,36,37].
One of these studies on the ACGME WTL showed that the mortality rates for nervous system disease and disorder patient population diverged between teaching and non-teaching institutions, with significantly higher mortality rates observed in teaching hospitals for 4 times of the next 7 years [7]. In 2009, Browne et al. [5] published a report on the ACGME WTL showing that the enforcement of WTL was associated with an accelerated rate of patient morbidity following treatment of hip fractures in teaching institutions. In contrast, Yaghoubian et al. [38] demonstrated that at a major public teaching hospital, bile duct injury rate and overall complication rate decreased after implementation of the ACGME WTL. A large retrospective analysis [23] in 2009 demonstrated slightly decreased mortality and morbidity among nationwide trauma patients in the US university hospitals after the 2003 ACGME WTL was enacted. Gopaldas et al. [13] reported decreased 30-day and 6-month mortality in cardiac surgery after the enactment of the WTL in the US hospitals.
In 2007, a literature by Volpp et al. [36] showed that the ACGME WTL was not associated with either significant worsening or improvement in mortality for Medicare patients in the first 2 years after implementation. Shonka et al. [34] in 2009 reported that institution of the ACGME WTL did not improve patient care as measured by the 30-day readmission rate, in-hospital mortality, and LOS. Rajaram et al. [32] demonstrated that implementation of the 2011 ACGME WTL was not associated with a change in general surgery patient outcomes in 2014. Another report published in 2014 showed there was no immediate improvement in Medicare patient mortality or readmission rate at 30 days after the 2011 ACGME WTL revision [30].
Although under the WTL of K-MHW, the mortality rate of sICH patients was higher than that prior to its enactment (17.3% vs. 12.6%) (Table 1), this study also indicated no clear effect of WTL (Table 1, 2, 3). In other words, enforcing the WTL of K-MHW did not significantly improve short-term treatment outcome.
The LOS with hospitalization cost (adjusted for severity) have been accepted as direct and indirect indicators of the quality of patient care, intra- and/or peri-operative complications, and comorbidity [1-3]. Babu et al. [3] claimed in 2014 that complication count significantly affected LOS. As well, in 2017 Alaraj et al. [1] analyzed spontaneous subarachnoid hemorrhage patients and reported that non-neurological complications such as pneumonia, respiratory failure, deep vein thrombosis, urinary tract infection were significant predictors of increased hospital LOS. And the hospital LOS has been regarded as one of the common metric of health care quality.
Although there might be many complex and/or unexpected factors that determined hospital LOS including health care delivery system, insurance status of patient, and healthcare-oriented insurance products in different countries, we agreed with the above concepts in principle. In our analysis, the hospital LOS after enforcement of the WTL was computed longer than before (20.2 days vs. 19.0 days) (Table 1), but this difference was not found to be significant.
Resident physician well-being, training and education
Although these subjects are beyond the scope of this study, enforcing the WTL for resident physician would strongly influence factors associated directly and/or indirectly with patient treatment outcome.
Drolet et al. [10] in their survey on the 2011 ACGME WTL, reported that the QoL of resident physician was the only factor that predicted improvement. A report published by an EU member country [35] on neurosurgical resident training and work/life balance, stated that over 95% of United Kingdom neurosurgical unit residents preferred traditional on- calls before the EU WTL (i.e., European Working Time Directive) since the traditional 24-hour on-call system provided more chances for clinical exposure. About 59% felt that they were more tired when doing duty shift work than oncalls and 64% found that the on-call system gave more useful spare time and more time to deal with family commitments. In summary, more neurosurgery registrars felt the shift system would be less safe, harmful to training and not favorable to work/life balance. Another report from the EU in 2019 presented by Jakola and Skoglund [18] demonstrated a strong decline in surgical cases over time, and trainees’ graduating after introduction of the EU WTL had chances of less surgical exposure. At seven years after the enforcement of the ACGME WTL, Jagannathan et al. [17] reported that the 80-hour work week of the ACGME WTL might adversely affect resident training. They also, stated that neurosurgical training program directors and chief residents believed that the 80-hour work week of the ACGME WTL made neurosurgical training and patient care more difficult. We believed that 2-year experience was very short period to academically and formally estimate the adequacy and/or efficacy of neurosurgical resident training.
Limitations of this study
There are numerous vulnerabilities in this study. First, there were some intrinsic limitations due to the retrospective nature of this study, including absence of data that were neither recorded nor tested. Second, we did not have the long-term treatment outcome and precise complication data. Then, we could not utilize and compare a number of complications before and after the enactment of K-MHW WTL. For example, we failed to compare non-neurologic complications between the pre- and post -WTL groups such as respiratory tract infections including pneumonia, respiratory failures, venous thrombosis including deep vein thrombosis of lower extremity, and urinary tract infections that should affect the short-term outcome and LOS since some patients’ medical records in the both groups were found to be deficient of those data. Third, this study looked at the experience of a single institute for relatively short-term, then this study results lack representativeness. Fourth, although the difference of sICH locations between the pre-WTL and post-WTL groups stood just on the borderline significance, since the difference in initial GCS scores in the both groups did not indicate to be significant, the authors regarded that the two groups were comparable. It however, might make some potential differences in our result and conclusion (Table 1). Fifth, each neurosurgeon, not neurosurgical trainee, have had three new night duties per a month in the emergency room (ER) from the middle of the study period. Even though it might not influence the management of sICH patient remarkably, it clearly made surgical decision-makings in sICH patients faster than the usual in ER. Therefore, this new night duty system for neurosurgeon as an educator in ER might modify our result. Finally, we decided to consider the hospital LOS as a proxy for the number and seriousness of complications during hospital treatment, and quality of patient care. And we did not separate hospital LOS into ICU and general floor LOS. A number of variables, however besides complications and quality of health care could have effects on the LOS. Therefore, our results warrant validation by further studies.
CONCLUSIONS
The contents of WTL are evolving, and the effects of enforcing WTL on the patient treatment outcome in the US and EU wherein WTL was implemented much earlier than in South Korea, are equivocal [5,11,13,l7,23,38]. Although a single institute’s experience of only 2 years, our present study showed that the WTL mandated by the K-MHW for resident physician did not significantly affect treatment outcomes and hospital LOS. On the other hand, the authors do not anticipate a better short-term outcome and shorter LOS if the K-MHW WTL goes back to the past. Further well-designed multi-institutional prospective studies whether the WTL enforcement exerts a positive influence on patient outcome in critical neurosurgical diseases such as sICH, are expected.
Notes
Disclosure
The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.